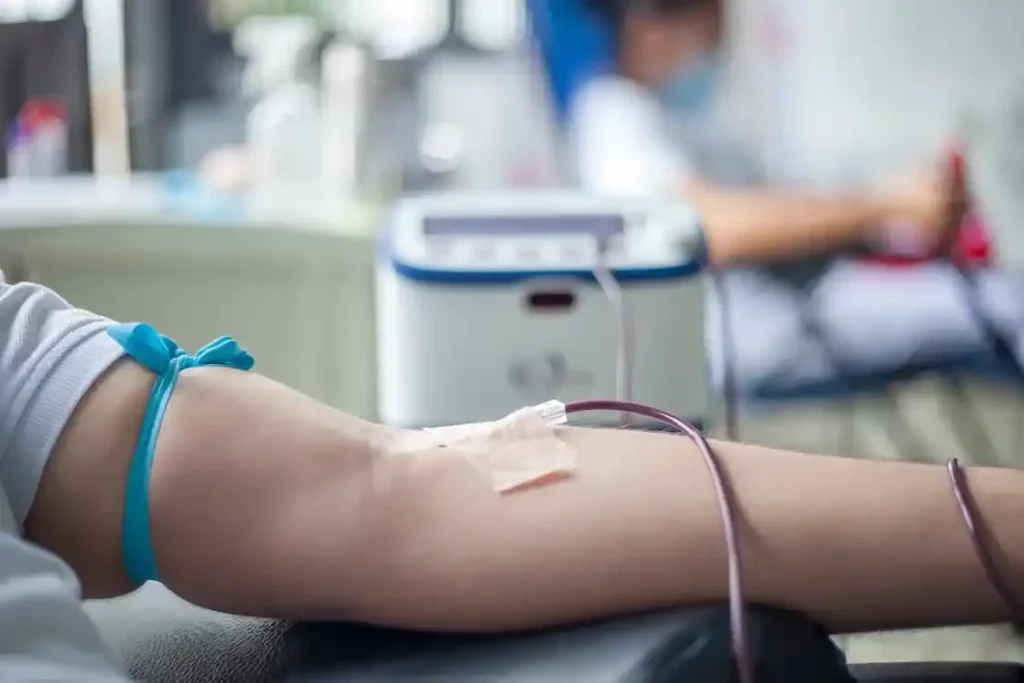
Kenya intends to implement blood automation technology to improve blood transfusion services and expand access to safe blood nationwide.
The Principal Secretary for Medical Services, Mr. Harry Kimtai, announced this initiative at the Africa Technology Day, hosted by Terumo Blood and Cell Technologies in Nairobi.
The automation technology, supplied by Terumo, aims to expedite blood component processing, enhance quality control, and minimize blood product wastage. Upon full deployment in Kenya’s regional blood centers, this technology is expected to extend red blood cell storage from approximately six to 45 days and enable frozen platelet storage for up to two years.
Addressing delegates from across Africa and representatives from Terumo Corporation Japan, Mr. Kimtai emphasized the vital role of blood in strengthening health systems. He noted that access to safe blood saves lives in critical situations, such as surgeries, childbirth, cancer treatment, and sickle cell disease management.
“Blood is a life-saving resource. Through automation, we will enhance the efficiency, quality, and sustainability of blood services in Kenya,” stated Mr. Kimtai.
Mr. Kimtai acknowledged advancements in blood technology adoption in countries like Zambia and Uganda and encouraged other African nations to follow suit. He also called for increased voluntary blood donation, moving away from reliance on high school donors, and urged support from the private sector, educational institutions, and the public.
The event gathered stakeholders to explore innovations in blood management, with Kenya aiming to lead in modernizing health systems for universal health coverage.
Voluntary Blood Donation: The Foundation of a Safe and Sufficient Life
Challenges and Solutions in Kenyan Blood Transfusion Services
Despite the life-saving nature of blood transfusions, many patients in Africa lack timely access to safe blood. African blood donation rates are significantly below the WHO recommendation of 10 donations per 1,000 people, with many countries collecting fewer than 5.
In Kenya, while the Kenya National Blood Transfusion Service collected 186,000 units of blood in 2024, the country’s annual requirement is estimated at 400,000 units, highlighting a significant shortfall.
Key challenges include
- Shortages due to obstetric hemorrhage, road accidents, and disease.
- Insufficient funding for personnel, equipment, and reagents.
- Inadequate infrastructure, including regional blood banks.
- Over-reliance on family replacement donors.
- Insufficient staffing at blood transfusion centers.
- Lack of public education on blood donation.
- Deficient healthcare professional training.
- High prevalence of transfusion-transmissible infections.
- Inadequate documentation and hemovigilance.
Potential solutions include
- Increased resource allocation.
- Investment in modern equipment and infrastructure.
- Promotion of voluntary blood donation.
- Strategies to attract and retain regular donors.
- Enhanced blood supply chain efficiency.
- Comprehensive quality management systems.
- Robust hemovigilance systems.
- Improved healthcare professional training.
- Effective screening and prevention of infections.
- Reduced barriers to access.
- Community stakeholder engagement.
- Comprehensive data collection and analysis.
- Fostering stakeholder collaboration.
WHO Efforts
The World Health Organization (WHO), aiming for 10 donations per 1,000 individuals, is collaborating with African nations to enhance blood safety and availability and has developed a Quality Management Programme for blood transfusion services.